The world was shocked after learning about Chadwick Boseman’s death from colorectal cancer. Unfortunately, his death from this disease was far too common (my friend died from colon cancer).
“Colorectal cancer is the second deadliest cancer in the country,” said Durado Brooks, M.D. vice president of prevention and early detection at the American Cancer Society. “This disease is ravaging the Black community and it is as important as ever that everyone has access to and is receiving the recommended screenings to prevent the disease or find it at an early, more treatable stage.”
Colorectal cancer disproportionately impacts the Black community, with among the highest rates of any racial/ethnic group in the U.S. African Americans are 20% more likely to get colorectal cancer and 40% more likely to die from it than other groups. Black men have the highest incidence rate.
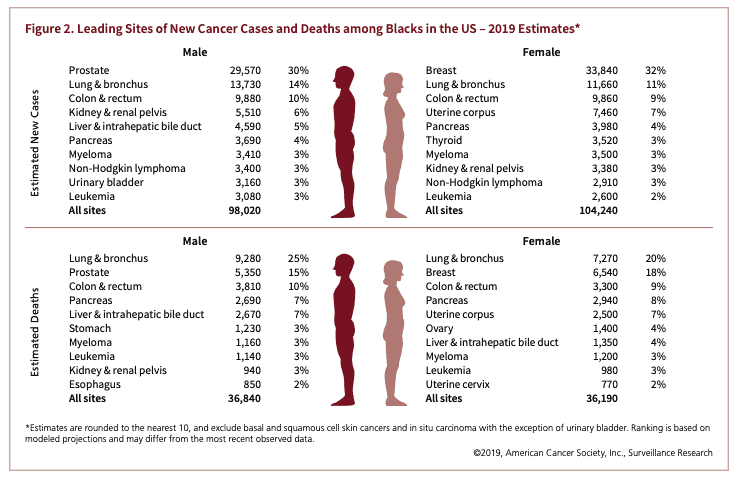
In addition, rates of colorectal cancer in younger age groups is rising. In 2020, 12% of colorectal cancer cases will be diagnosed in people under 50 – about 18,000 cases. Since the mid-1980’s, adults age 20-39 have experienced the steepest increase in colorectal cancer rates.
The American Cancer Society recommends that people with average risk begin regular screening at age 45.
Test Options for Colorectal Cancer Screening
Screening can prevent colorectal cancer by finding and removing growths, called polyps, in the colon and rectum before they become cancer. Several test options are available for colorectal cancer screening:
Stool-based tests
- Highly sensitive fecal immunochemical test (FIT) every year
- Highly sensitive guaiac-based fecal occult blood test (gFOBT) every year
- Multi-targeted stool DNA test (mt-sDNA) every 3 years
Visual (structural) exams of the colon and rectum
- Colonoscopy every 10 years
- CT colonography (virtual colonoscopy) every 5 years
- Flexible sigmoidoscopy (FSIG) every 5 years
No matter which test you choose, the most important thing is to get screened. Talk to your healthcare provider about which tests might be good options for you.
Risk Factors for Colorectal Cancer
Those with higher risk should consider – with their physician – earlier screening. Higher risk factors include:
- Family history of colorectal cancer or certain types of polyps
- Personal history of colorectal cancer or certain types of polyps
- Personal history of inflammatory bowel disease (ulcerative colitis or Crohn’s disease)
- Known family history of a hereditary colorectal cancer syndrome such as familial adenomatous polyposis (FAP) or Lynch syndrome (also known as hereditary non-polyposis colon cancer or HNPCC)
- Personal history of radiation to the abdomen (belly) or pelvic area to treat a prior cancer
In addition, anyone with abdominal or gastro-intestinal symptoms such as a change in bowel habits that lasts for more than a few days; rectal bleeding; blood in the stool; cramping or abdominal pain; weakness and fatigue; or unintended weight loss should consult with their doctor.
Symptoms of Colorectal Cancer
Many of the symptoms of colorectal cancer can also be caused by something that isn’t cancer, such as infection, hemorrhoids, irritable bowel syndrome, or inflammatory bowel disease.
Still, if you have any of these problems, it is a sign that you should go to the doctor so the cause can be found and treated if needed:
- A change in bowel habits, such as diarrhea, constipation, or narrowing of the stool, that lasts for more than a few days
- A feeling that you need to have a bowel movement that is not relieved by doing so
- Rectal bleeding
- Dark stools, or blood in the stool
- Cramping or abdominal (belly) pain
- Weakness and fatigue
- Unintended weight loss
When colorectal cancer does turn out to be the cause, symptoms often appear only after the cancer has grown or spread. That’s why it’s best to be tested for colorectal cancer before ever having any symptoms. When found early, before it has spread, the 5-year relative survival rate is 90%.
For more information or to speak with someone about colorectal cancer and its effects on the Black community, experts and physicians from the American Cancer Society can provide interviews, information, and valuable resources.
Tweet us @mochamanstyle or leave a comment on our Facebook Page to share your thoughts on this article. Follow us on Instagram @mochamanstyle

Frederick J. Goodall is the Editor-in-Chief of Mocha Man Style, media spokesperson, event host, photographer, and a top social media influencer in Houston, TX. He likes to write about fashion, cars, travel, and health.

